If you have a medium-dark or dark skin type and are treating melasma with the Kligman formula, or have been prescribed it, it's important to understand what actually happens to your skin during that treatment.
The Kligman formula has been the gold standard for melasma treatment for decades. But one of the fundamental principles of modern dermatology is that not all protocols work equally well on all skin types. For dark skin types (III-VI on the Fitzpatrick skin type scale), this formula presents specific risks that can not only reduce its effectiveness but also lead to an active worsening of pigmentation.
The Kligman formula has been the gold standard for melasma treatment for decades. But one of the fundamental principles of modern dermatology is that not all protocols work equally well on all skin types. For dark skin types (III–VI on the Fitzpatrick skin type scale), this formula presents specific risks that can not only reduce its effectiveness but also lead to an active worsening of pigmentation.
How melanocytes work in dark phototypes
To understand why the Kligman formula is problematic in dark skin types, we must first understand how melanocytes function in this skin type.
Dark phototypes (Fitzpatrick IV-VI) do not produce more melanin because they have more melanocytes: the number of melanocytes is similar in all phototypes. The difference lies in activity. Melanocytes in dark phototypes are naturally more active, produce larger melanosomes, and distribute them more efficiently to the superficial layers of the skin.
This has a direct consequence: any inflammatory stimulus, even moderate, can result in a significant increase in melanin production. Irritation, heat, microtrauma, allergic reactions: in a light skin type, these events cause temporary redness. In a dark skin type, the same event can leave a pigmented spot that persists for weeks or months.
This mechanism is called post-inflammatory hyperpigmentation (PIH), and it underlies the Kligman formula paradox in dark skin types: a treatment designed to lighten dark spots can, through the irritation it causes, generate new ones or intensify existing ones. To learn more about the mechanism of PIH, you can consult the article onpost-laser hyperpigmentation or the guide on how to distinguish PIH from melasma.
What is the Kligman formula and how does it work?
The classic Kligman formula combines three active ingredients: hydroquinone (4–5%), tretinoin (0.1%), and a corticosteroid (usually fluocinolone acetonide or hydrocortisone). Each component has a specific role:
Hydroquinone inhibits tyrosinase, the enzyme responsible for melanin synthesis. Tretinoin accelerates cell turnover and increases hydroquinone penetration. The corticosteroid reduces the local inflammation caused by the first two components, indirectly limiting the pigmentary response that irritation could otherwise trigger.
In theory, the combination is synergistic. In practice, for dark skin types, each component carries a specific risk profile that can outweigh the benefits. For a complete overview of the formula, you can read the article on the Kligman formula: composition and safe alternatives or the comparison between modern and traditional approaches.
Why Kligman's formula worsens melasma in dark skin types
1. Tretinoin: irritation and paradoxical PIH
Tretinoin is a first-generation retinoid that acts on the RAR nuclear receptors, accelerating epidermal cell turnover and altering keratinocyte differentiation. In Kligman's formula, it is used to accelerate cell turnover and increase hydroquinone penetration. This mechanism, however, almost inevitably leads to local irritation in the first few weeks of use.
Tretinoin irritation manifests as redness, scaling, burning, and sometimes swelling. In fair skin types, these effects are often tolerable and temporary. In dark skin types, each bout of irritation activates melanocytes in the treated area and can cause post-inflammatory hyperpigmentation. The result is what dermatologists call "paradoxical PIH": melasma is treated, but a superimposed PIH is triggered, making the skin even darker.
During tretinoin treatment, the skin undergoes a process of accelerated cell renewal that temporarily reduces the thickness of the stratum corneum. This thinning reduces the skin's natural physical protection from external agents, including UV radiation. The practical result is that treated skin is more vulnerable to sun damage than baseline, regardless of the season. Applying SPF 50 sunscreen every morning is therefore not an adjunct to treatment: it is a necessary condition for the treatment to not produce the opposite effect to the desired one. For a more in-depth comparison of tretinoin and more tolerable alternatives, see the article on tretinoin vs. new-generation retinoids.
2. Hydroquinone: risk of rebound and exogenous ochronosis
Hydroquinone has been banned in Europe for free cosmetic use since 2001 (EC Regulation 1223/2009), and can only be used in prescription formulations. The reasons for this restriction are based on clinical evidence.
The first risk is pigmentary rebound: after stopping hydroquinone, especially if treatment has been prolonged, melasma may recur, more intense than the initial situation. Melanocytes, suppressed for weeks or months, react with a compensatory overproduction of melanin.
The second risk, rarer but very serious, is exogenous ochronosis from hydroquinone.
Exogenous ochronosis is a dermatological condition caused by prolonged use of high-concentration topical hydroquinone. It manifests as grayish or blue-black spots in the treated areas, often with a granular appearance that dermatologists describe as "caviar" or "banana." They typically appear on the cheeks and malar areas, the same areas affected by the melasma being treated. The result, paradoxically, is darker, deeper pigmentation, and a different color than the original pigment.
The mechanism is biochemical. Hydroquinone, degrading in the skin, produces intermediate compounds that polymerize in the dermis and deposit in collagen fibers as ochronotic pigment. These deposits are not melanin and do not respond to traditional depigmenting agents: they are structurally integrated into the dermal tissue and are not eliminated by epidermal cell turnover. For this reason, exogenous ochronosis is considered virtually irreversible with standard cosmetic treatments.
Cases documented in the literature predominantly involve women with dark skin types (IV–VI) who had used hydroquinone-based products for periods exceeding 6–12 months, often without medical supervision and sometimes with products purchased outside of regulated channels (where concentrations can be significantly higher than the European limit). This does not mean that the condition is impossible with low concentrations, but the risk increases directly with the duration and concentration of treatment.
In darker skin types, the risk is greater for a structural reason: melanocytes are more reactive to any local biochemical alteration and produce larger melanosomes, distributed more efficiently in the superficial layers. The accumulation of hydroquinone compounds in the dermis occurs similarly in all skin types, but the overlapping pigmentary response (local inflammation, melanocyte activation) amplifies the visible damage in darker skin types.
From a practical standpoint, exogenous ochronosis cannot be treated with creams. Dermatological protocols include Q-switched lasers, deep peels, and, in the most severe cases, combined approaches. None of these guarantee complete resolution. It is this irreversibility, rather than the frequency of the phenomenon, that makes exogenous ochronosis a central issue in the debate about hydroquinone in dark skin types. To learn more about the specific risks of hydroquinone and the alternatives available in Europe, the dedicated article explains why hydroquinone is banned in Europe and what alternatives exist.
3. Corticosteroid: skin atrophy and rebound effect
The corticosteroid in the Kligman formula is used to modulate the irritation caused by tretinoin and hydroquinone. However, prolonged use of topical corticosteroids carries its own risks, regardless of skin type.
The most documented effect is skin atrophy: the corticosteroid reduces the thickness of the dermis, making the skin thinner, more fragile, and more permeable to external agents. Telangiectasias (visible dilated capillaries) may appear in the treated areas, and the skin tends to lose elasticity.
The second problem is the rebound effect upon discontinuation: the corticosteroid suppresses local inflammation during treatment, but when it is stopped, the inflammation can recur in an acute form, triggering a new cycle of PIH in dark skin types.
4. The formula is not sustainable in the long term
Melasma is a chronic condition. Unlike some forms of PIH, which tend to regress spontaneously with sunscreen, melasma requires ongoing maintenance for months or years.
Kligman's formula is not suitable for this type of use. Dermatologists recommend limited cycles (typically 8–12 weeks) with breaks between cycles, precisely because of the risks associated with hydroquinone and corticosteroids. But a fragmented approach is not compatible with the chronic nature of melasma: between cycles, sun exposure and hormonal factors continue to fuel melanogenesis.
In this sense, dark skin types are at a particularly disadvantage: they require more continuous treatment than light skin types, but they tolerate the irritating components of the classic formula worse.
The Irritation Paradox: The More You Treat, the Worse It Gets
This is the point that often surprises those who begin treatment with the Kligman formula and expect rapid results.
In the first few weeks, tretinoin causes irritation. This irritation leads to localized inflammation. This inflammation activates melanocytes in the treated areas. Melanocytes produce melanin in response to stress. The result is that the spot, instead of lightening, temporarily deepens.
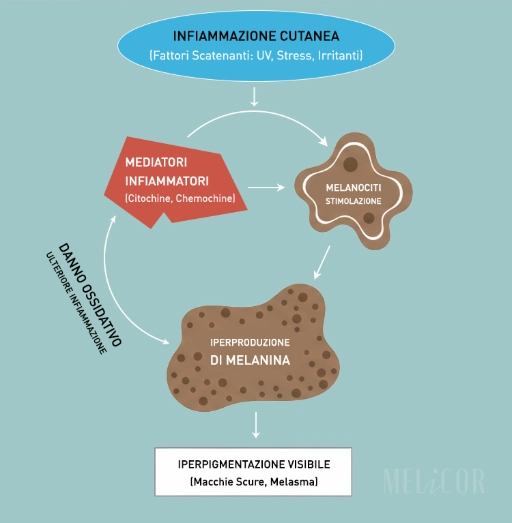
Many people with dark skin types stop treatment at this stage, interpreting the worsening as an allergic reaction or a sign that the product isn't working. In reality, they're experiencing the exact mechanism that makes Kligman's formula unsuitable for skin types IV–VI: the path to results involves irritation that dark skin types can't tolerate without pigmentation consequences.
The alternative isn't to increase the dose or persist: it's to change your approach with depigmenting active ingredients that work without triggering this cycle. For a more comprehensive assessment of which ingredients may aggravate melasma rather than treat it, it's helpful to read the guide on ingredients to avoid if you have melasma.

What to use instead: alternatives for dark skin types
Research in recent years has produced depigmenting active ingredients with a safety profile significantly superior to the classic formula, specifically tested and indicated for dark skin types.
Tranexamic acid is currently one of the most studied active ingredients for melasma and PIH. It works by interrupting the communication between keratinocytes and melanocytes, which leads to overproduction of melanin, without directly inhibiting tyrosinase (as hydroquinone does) and without causing irritation. It is suitable for prolonged use and is also effective for skin types IV–VI. You can learn more about its mechanism of action in the ingredient information for tranexamic acid.
Oleyl adapalenate is a third-generation retinoid that accelerates cell turnover with significantly better tolerability than traditional tretinoin. It acts on the nuclear receptors RAR-β and RAR-γ, a more selective receptor profile than tretinoin, which also binds to RAR-α. This selectivity results in less local irritation and less impact on the stratum corneum compared to first-generation retinoids. It is particularly suitable for sensitive skin types or those who have previously reacted to tretinoin. Further information is available in the Oleyl adapalenate.
Niacinamide works through a different mechanism: it reduces the transfer of melanosomes from melanocytes to keratinocytes, thus limiting the distribution of melanin in the superficial layers of the skin. It also has an anti-inflammatory effect, making it particularly suitable for skin types prone to PIH. Product information available on niacinamide.
Tetrahydrocurcumin is a turmeric derivative with powerful antioxidant and tyrosinase inhibitor properties, without the risks of hydroquinone. It works by blocking melanin synthesis upstream, with a documented safety profile for long-term use. For more information, see the tetraidrocurcumin.
Lumicor combines tranexamic acid, cetyl tranexamate mesylate, and oleyl adapalenate in a formulation specifically designed for the prevention and treatment of post-inflammatory hyperpigmentation, without hydroquinone or corticosteroids. It acts simultaneously on multiple melanogenesis pathways and is suitable for continuous use on dark skin types.

The practical protocol for phototypes III–VI
An effective protocol for melasma in dark skin types is divided into three phases.
Phase 1: Protection (year-round, no exceptions). Daily sun protection is an absolute must. Without consistent SPF, no depigmenting agent will produce long-lasting results. SPF 50 sunscreen should be applied every morning, even in winter and on cloudy days. For melasma, a tinted version is preferable: SPF 50 tinted sunscreen contains iron oxides that also filter high-energy visible (HEV) light, which can stimulate melanogenesis independently of UV rays. For dark skin types who prefer an SPF 30 formulation with mineral filters, SPF 30 mineral sunscreen offers a daily base that is tolerated even in the summer. For a complete overview of the role of SPF in treating melasma, the guide on SPF and Melasma: Why Mineral Protection is Essential is available.
Phase 2: Depigmenting treatment. The application of a hydroquinone-free depigmenting agent should be introduced gradually, starting with 2–3 weekly applications in the evening and gradually increasing as tolerated. Dark skin types benefit from a "slow and steady" approach: slower results but without the risk of paradoxical PIH. The hydroquinone-free melasma treatment protocol offers a step-by-step guide on how to build this phase.
Phase 3: Maintenance. Once visible improvement is achieved (typically after 2–4 months), the maintenance phase involves continued use of SPF and less frequent applications of the depigmenting product. Melasma cannot be "cured": it is managed. A proper maintenance approach can significantly reduce recurrences, especially in the summer months.
For dark skin types who have undergone or are planning laser procedures, it is also important to consult the guide on Nd:YAG laser hair removal for dark skin types: the choice of laser type is important to reduce the risk of post-procedural PIH, which in skin types IV–VI can overlap with existing melasma.
Frequently Asked Questions
Can the Kligman formula work on dark skin types?
In some cases, under strict dermatological supervision, the Kligman formula is still prescribed for skin phototypes IV–VI, but with modified protocols (lower concentrations, short cycles, frequent monitoring). In private cosmetic practice, however, the risk profile of the classic formula is difficult to manage without medical supervision. Modern alternatives offer a more favorable risk/benefit ratio for self-use.
How long does it take to see results with hydroquinone alternatives?
The timeframes are generally longer than those for the Kligman formula: 8–12 weeks for the first visible improvements, 4–6 months for consolidated results. However, the progression is more stable and without the risk of rebound upon discontinuation.
Is tinted SPF really necessary for melasma, or is clear enough?
For melasma, tinted SPF with iron oxides offers an additional benefit: it filters high-energy visible (HEV) light, which recent studies have linked to the stimulation of melanogenesis. For dark skin types and recalcitrant melasma, this additional protection can make a practical difference.
Can I use depigmenting active ingredients after a laser procedure?
Not immediately. In the acute post-laser phase, the priority is to repair the skin barrier and reduce inflammation. Only once the recovery phase is complete can depigmenting agents be gradually introduced. Each type of laser has different recovery times: for the differences between the main technologies, it's helpful to read about CO₂ lasers and erbium lasers: differences, recovery, and skin care comparison.
How do I know if I have melasma or PIH?
The two types of hyperpigmentation have different mechanisms, distribution, and response to treatment. An accessible diagnostic guide is available in the article How to Tell if You Have PIH or Melasma.
How is exogenous hydroquinone ochronosis recognized?
Exogenous ochronosis presents as grayish or blue-black spots with a granular appearance, distributed in the same areas treated with hydroquinone (typically the cheeks and malar area). Unlike melasma, the spots have an abnormal color, tending towards grayish or bluish, and do not respond to standard depigmentation treatments. A definitive diagnosis requires dermatoscopy. If this condition is suspected, hydroquinone use should be discontinued immediately and a dermatologist consulted.
Scientific references
- Davis EC, Callender VD. Postinflammatory hyperpigmentation. J Clin Aesthet Dermatol. 2010.
- Ogbechie-Godec OA, Elbuluk N. Melasma: an Up-to-Date Comprehensive Review. Dermatol Ther (Heidelb). 2017. Lim JT. Treatment of melasma using kojic acid in a gel containing hydroquinone and glycolic acid. Dermatol Surg. 1999.
- Passeron T et al. Melasma and photoprotection. J Am Acad Dermatol. 2013.
- Grimes PE. Management of hyperpigmentation in darker racial ethnic groups. Semin Cutan Med Surg. 2009.