Post-laser pigmentation is one of the most common concerns of those approaching laser facial treatment. It sometimes appears a few weeks after the procedure, completely unexpectedly: the skin appears improved, then brown spots appear where the skin was previously even. This is not an uncommon exception. It is a predictable biological response that can, in most cases, be effectively prevented.
This guide describes the physiological causes of post-inflammatory hyperpigmentation (PIH), individual risk factors, and a structured protocol to minimize the likelihood of its occurrence.
Why laser can cause hyperpigmentation
The laser acts on the skin tissue through thermal or photonic energy. This energy, regardless of the method used, triggers a local inflammatory response that is an integral part of the regenerative process. The problem arises from what happens at the level of melanocytes, the cells responsible for producing melanin.
Under normal conditions, melanocytes produce melanin in response to UV rays as a protective mechanism. When the skin is subjected to an inflammatory stimulus, such as that produced by laser treatment, melanocytes can activate the same mechanism in an abnormal and localized manner. The result is excess melanin that is deposited in the superficial layers of the skin, forming brown or gray-brown spots in the weeks following the procedure.
This process is called post-inflammatory hyperpigmentation, or PIH. It is not an allergic reaction, nor does it cause permanent damage in most cases. It is a biological response that can be modulated by addressing the factors that amplify it, particularly sun exposure and a lack of skin barrier protection during the critical stages of recovery.
The article dedicated topost-laser hyperpigmentation delves into the physiology of this process and the treatment options once PIH has already appeared.
Who is really at risk?
The risk of developing PIH after laser treatment is not the same for everyone. Two factors significantly increase the likelihood: skin phototype and the type of procedure.
I skin phototypes most at risk are those from III to VI according to the Fitzpatrick skin type scale, namely olive, Mediterranean, Middle Eastern, Latin, and dark-skinned skin. In these phototypes, melanocytes are already structurally more active and react more intensely to inflammatory stimuli. This doesn't mean that people with phototypes I or II are completely immune, but the likelihood is significantly lower.

When it comes to procedures, the risk varies considerably. Fractional ablative lasers, particularly fractional CO₂ lasers, produce a more intense and prolonged inflammatory response and carry a higher risk of PIH than non-ablative lasers. Laser hair removal methods, such as 808 nm diode or alexandrite, have a lower but not zero risk profile, especially for darker skin types and for summer treatments.
A third determining factor is the patient's behavior in the weeks following the procedure. Unprotected sun exposure during this phase is the main trigger for PIH, regardless of skin type.
When to start: the 4 phases of the protocol
PIH prevention doesn't start the day after laser treatment. It begins before and continues for weeks afterward. The protocol is structured into four distinct time phases, each with specific objectives.
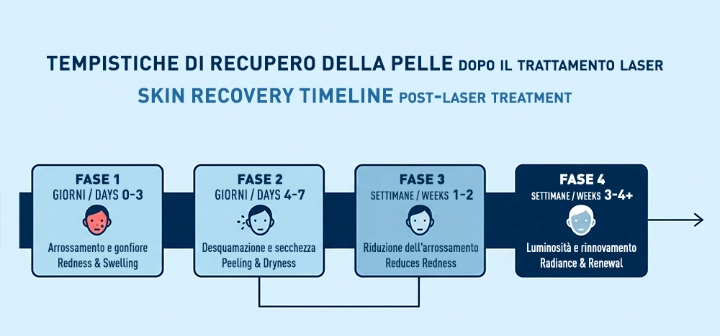
Phase 1: Preparation before the procedure (2 weeks before)
In the 14 days preceding treatment, the goal is to reduce baseline melanocyte activity and bring the skin into the best possible condition to cope with the procedural trauma.
At this stage, in consultation with your doctor, you may want to consider using low-concentration depigmenting ingredients such astranexamic acid or niacinamide. Both reduce the transfer of melanin to keratinocytes through different and complementary mechanisms, without irritating the skin before the procedure.
It is essential to avoid any direct sun exposure in the two weeks preceding the procedure and to discontinue the use of retinoids or exfoliating acids at least 5 days beforehand, to reduce skin sensitivity.
Phase 2: Acute phase (days 1 to 7)
In the first seven days after laser treatment, the skin is actively inflammatory. Redness, swelling, and a sensation of heat or burning are normal and part of the regenerative process. Any aggressive intervention during this phase, from mechanical exfoliation to the use of potent active ingredients, risks prolonging the inflammation and increasing the risk of PIH rather than reducing it.
At this stage, the goal is not to correct, but to protect. Cleansing should be done with a product formulated for sensitive and reactive skin, which removes impurities without altering the rebuilding hydrolipidic film. Immediately afterward, a repairing cream based on soothing and highly hydrating ingredients such ashyaluronic acid helps maintain transepidermal hydration and support the healing process.
Sunscreen is mandatory during this phase, even in cloudy weather or when spending most of your time indoors. UVA rays penetrate glass and reach the skin even in the absence of direct sunlight. Using a broad-spectrum sunscreen with an SPF of 50, preferably mineral-based, is the first and most important measure for preventing PIH.
Phase 3: Re-epithelialization (days 7 to 21)
Once the peeling is complete and the skin returns to a normal consistency, you can gradually begin introducing ingredients with preventative depigmenting properties. This is the most important window of opportunity to address nascent PIH, which can still be prevented before it becomes visible.
Tranexamic acid and niacinamide remain the ingredients of choice in this phase: they act upstream of the pigmentation cascade, reducing melanin synthesis and transfer without irritating skin that is still recovering. Tolerability during this phase takes precedence over potency: a well-tolerated, moderately concentrated active ingredient is better than a highly concentrated one that causes redness.
Sun protection remains unchanged: SPF 50 every morning, reapplying every two hours in case of direct exposure.
Phase 4: Maintenance (months 1 to 3)
In the two months following the completion of re-epithelialization, the skin is structurally vulnerable to pigmentation, and melanogenesis can easily reactivate in response to even minimal stimuli. Maintaining this phase determines the stability of the result over time.
The protocol for this phase includes the continued use of a depigmenting agent in the evenings and sunscreen in the morning, a must-have habit. If the first areas of hyperpigmentation appear, it's time to introduce a specific formulation for the treatment of PIH and melasma, with a higher concentration of active ingredients.
The ingredients that make the difference
The scientific literature on the treatment and prevention of PIH identifies some ingredients with a superior efficacy/tolerability profile, particularly suitable for use in the post-laser phase.
Tranexamic acid works by inhibiting the interaction between keratinocytes and melanocytes, reducing inflammation-induced melanin production. It is one of the most studied ingredients for the prevention of post-procedural PIH and is tolerated even by sensitive skin in the weeks following laser treatment.
Niacinamide (vitamin PP or B3) inhibits the transfer of melanosomes from melanocytes to keratinocytes, the final step in the formation of spots. Its anti-inflammatory action makes it particularly useful in the transition between the acute phase and re-epithelialization.
Silymarin, an antioxidant derived from milk thistle, complements the action of the depigmenting ingredients by counteracting oxidative stress that amplifies the post-inflammatory melanogenic response.
The combined use of these ingredients allows you to act on multiple points of the pigment cascade simultaneously, increasing the overall effectiveness of prevention.
3-step protocol: from acute phase to maintenance

Step 1: Gentle cleansing
After laser treatment, conventional cleansers can further disrupt an already compromised skin barrier, prolong inflammation, and increase sensitivity. It's essential to use a product specifically formulated for recovering skin, with a physiological pH and ingredients that support the rebuilding of the hydrolipidic film. A gentle cleansing gel for sensitive skin with a soothing effect is the appropriate choice from the acute phase until complete re-epithelialization.
Step 2: Repair and Hydrate
During the acute phase and the first week, the cream should primarily support the recovery of the barrier, reduce inflammatory discomfort, and maintain hydration. A post-laser repair cream formulated with soothing and regenerating ingredients meets these requirements without clogging pores or interfering with healing processes. For body treatments, such as laser hair removal, a specific soothing formulation, such as the soothing cream after laser hair removal, is more suitable.
Step 3: Mineral sunscreen
Sunscreen after laser treatment is not an afterthought. It is a physiological necessity that allows no exceptions or derogations due to cloudiness, season, or individual habits. Mineral sunscreens, based on zinc oxide and titanium dioxide, are preferable to chemical sunscreens in the post-procedure phase because they act by physical reflection without penetrating inflamed skin and without the risk of sensitization.
An SPF 50 facial sunscreen for sensitive skin provides maximum protection during the most critical weeks. In subsequent phases, or for daily use during maintenance, an SPF 30 mineral sunscreen can be a valid alternative during the season with lower solar radiation.
Step 4: Active prevention of pigmentation
Starting in the second week after laser treatment, when re-epithelialization is underway, a specific formulation for the prevention and treatment of pigmentation can be introduced. A cream containing tranexamic acid, niacinamide, and antioxidant ingredients targets the mechanisms that lead to the formation of spots, blocking the process before it becomes visible. A hydroquinone-free anti-hyperpigmentation cream can be introduced at this stage and continued throughout the maintenance period.
The most common mistakes to avoid
Post-laser PIH, in most cases where it occurs, is the consequence of behaviors that amplify the inflammatory response or that expose the skin to pigmentogenic stimuli in the most critical phases of recovery.
Sun exposure without adequate protection is the most common and most damaging mistake. Even brief exposure without SPF in the first three weeks can be enough to trigger a melanogenic response that is difficult to correct later.
Resuming the use of exfoliating acids or retinoids too soon is another common cause. These ingredients, while effective under normal conditions, irritate recovering skin and amplify inflammation, increasing the risk of PIH rather than reducing it. The general rule of thumb is to wait at least four weeks, or until your doctor approves.
Using hot water to wash your face in the first two weeks, using a sauna or engaging in intense physical activity that causes profuse sweating, and using perfumed or alcohol-based products all prolong irritation and slow down the barrier's recovery.
Finally, interrupting the prevention protocol too early, often after just a few days because the skin appears to have already healed, is a mistake that underestimates the true time window of PIH risk, which extends for two to three months after the procedure.
Melicor post-laser kit
For those who have undergone a fractional CO₂ laser or photorejuvenation treatment, the post-CO₂ laser facial kit combines products for the acute and re-epithelialization phases in a ready-to-use protocol. For laser hair removal treatments, the complete post-laser hair removal kit is formulated to meet the specific body care needs in the weeks following the session.
Frequently Asked Questions
When can I start using an anti-blemish cream after laser?
Generally speaking, a specific formulation for pigmentation prevention can be introduced starting from the second week after laser treatment, when peeling is complete and the skin has returned to a normal consistency. Before this stage, the use of potent active ingredients can irritate the skin and increase the risk of PIH. The exact timing depends on the method used and the individual's recovery process: it's always helpful to confirm with the doctor who performed the procedure.
Mineral or chemical SPF after laser: which one to choose?
If PIH has already appeared, the treatment protocol differs from prevention: it requires higher concentrations of active ingredients and longer-term use. The article onpost-inflammatory hyperpigmentation describes treatment options in detail. If the spots have already formed, it's advisable to consult a dermatologist to assess the depth of pigmentation and the most appropriate strategies.
Does this protocol apply to all types of lasers?
The protocol applies to all laser treatments with an inflammatory effect on the skin, including fractional CO₂ lasers, erbium lasers, non-ablative lasers, and laser hair removal treatments. The intensity of the necessary prevention varies: ablative methods require a more rigorous and prolonged protocol than non-ablative methods or hair removal. The physician performing the procedure can specify specific timeframes based on the type of laser and the parameters used.
How long is the PIH risk period?
The period of greatest vulnerability extends for the first three to four weeks after laser treatment, but the risk does not completely disappear in the following three months, especially for darker skin types and intensive ablative procedures. Sun protection must be maintained rigorously for at least three months after treatment, and ideally as a lifelong habit for those with skin type III or higher.