The CO₂ laser is one of the most effective tools in aesthetic dermatology: it acts deeply, stimulates collagen production, and produces visible results after just one or two sessions. Among the lasers currently in use, it is also the one with the greatest potential to cause dark spots in the weeks following treatment. This complication is called post-inflammatory hyperpigmentation (PIH) and is preventable, provided you know how and when to intervene.
Prevention doesn't start after laser treatment. It starts before.
Why CO₂ laser can cause dark spots
The CO₂ laser is an ablative laser: it physically removes the superficial layers of the skin through controlled thermal vaporization. This action is precise and effective, but inevitably triggers an intense inflammatory response in the dermis and surrounding epidermis.
This is where the problem arises. Melanocytes, the cells responsible for producing melanin, are extraordinarily sensitive to inflammatory signals. When tissue is damaged, the body releases a cascade of mediators, including prostaglandins, interleukins, and other factors, which stimulate melanocytes to increase their production. The result, in some cases, is a localized overproduction of melanin, which deposits irregularly and produces the dark spots typical of PIH.
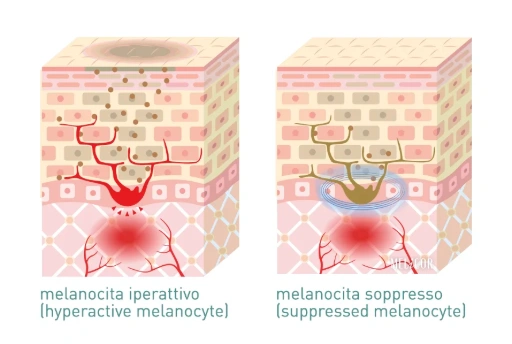
The risk is not the same for everyone. Darker skin phototypes (Fitzpatrick III–VI) have naturally more reactive melanocytes, and the inflammatory response tends to produce more intense melanogenic stimulation. For phototypes I and II, the risk exists but is significantly lower. For phototypes V and VI, the CO₂ laser requires a very careful medical evaluation: in these cases, the risk-benefit ratio may guide you towards non-ablative alternatives.
Pre-procedure preparation: the step that changes everything
One of the most effective strategies for reducing the risk of PIH after CO₂ laser is skin preparation in the weeks leading up to treatment. The goal is to reduce the baseline reactivity of melanocytes before the laser even takes effect, thus attenuating the pigmentary response that can follow inflammation.
This approach is based on the use of melanosuppressant agents applied topically in the pre-procedural period.
Skin types I and II: The preparation protocol typically lasts two weeks. In this case, melanocyte reactivity is limited, and the short pre-treatment cycle is sufficient to significantly reduce the risk.
Skin types III and IV: Preparation should begin at least four weeks before the procedure. More reactive melanocytes require longer conditioning to respond effectively to melanogenesis inhibitors.
Agents indicated in this phase includetranexamic acid and niacinamide, which act on distinct mechanisms of melanin synthesis without irritating the skin, a key requirement for an ablative procedure. Lumicor combines both molecules in a single formulation, making it suitable for the pre-laser preparation phase.
Pre-procedural preparation should always be agreed upon with the doctor performing the treatment, as some active ingredients require suspension in the days immediately preceding the procedure.
Complete protocol: from preparation to maintenance
weeks
before
Preparation
Conditioning of melanocytes
Apply a topical melanogenesis inhibitor to reduce melanocyte reactivity before the procedure.
Skin types I–II: 2 weeks.
Skin types III–IV: 4 weeks.
Associated product: Lumicor.
Acute phase
Barrier protection
Gentle cleansing, a repairing cream to reduce inflammation, and mineral SPF from the very first days. No melanosuppressant active ingredients are used until complete re-epithelialization.
Related products: Enzyclean · Epicalm Plus · SPF 50
4–8
Maintenance
Melanogenesis inhibition + UV protection
After re-epithelialization (days 7–10), introduce melanosuppressant agents. Mineral SPF every morning for the entire recovery period. Related products: Lumicor SPF 50
Risk factors: what increases the likelihood of PIH
In addition to skin type, there are other factors that significantly increase the likelihood of developing irregular pigmentation after CO₂ laser treatment:
Sun exposure during recovery. UV rays directly stimulate melanocytes and amplify the pigmentary response already activated by inflammation. Even brief, unintentional exposure, such as walking in full sun without protection, is enough to trigger or worsen PIH in the weeks following laser treatment.
Inadequate cleansing. The use of harsh or perfumed cleansers during the acute phase further alters the skin barrier, prolongs the inflammatory process, and consequently maintains melanocyte stimulation for longer.
Forced removal of scabs. The scabs that form in the days following ablative laser treatment serve a specific protective function. Removing them prematurely causes microtrauma, increases the risk of infection, and creates the conditions for uneven pigmentation.
Lack of adequate sun protection. Applying a standard sunscreen after laser treatment is not sufficient. Post-ablative skin requires high-factor protection with mineral filters, which physically reflect UV light without triggering chemical reactions on the affected skin surface.
History of melasma. Those who have had previous episodes of melasma or hormonal hyperpigmentation have more structurally reactive melanocytes. In these cases, prevention requires a more structured approach both before and after the procedure.
The 3-step post-CO₂ laser protocol
Step 1: Protect the barrier (days 1–7)
In the first 24–72 hours after fractional CO₂ laser treatment, the skin is erythematous, edematous, and lacks a functional barrier. The goal at this stage is not yet to inhibit melanogenesis, but to limit inflammation and protect the skin while it regenerates.
A specific cleanser for sensitive and reactive skin with no harsh surfactants is the foundation of any proper post-laser routine. Cleansing keeps the area clean without removing residual barrier lipids or irritating the regenerating tissue.
For active barrier repair, Epicalm Plus Repair Cream is formulated for the post-ablative phase: it targets local inflammation, reduces itching, and supports regeneration without occlusive or comedogenic ingredients. Reducing inflammation during this phase has a direct effect on preventing PIH: fewer inflammatory signals mean less stimulation of melanocytes.
Sun protection begins in the first few days. Even in the absence of direct sun exposure, ambient UV light is enough to trigger the pigmentation response in compromised skin. A light SPF 50 face cream a light formulation is the most suitable choice.
Step 2: Inhibit melanogenesis (from day 7–10)
Once re-epithelialization is complete, generally between the seventh and tenth day after fractional CO₂ laser treatment, it's time to introduce melanosuppressant agents. Doing so beforehand is not only unnecessary: on skin that's still healing, it can be irritating and counterproductive.
Lumicor combines tranexamic acid, cetyl tranexamate mesylate, niacinamide, tetrahydrocurcumin, and silymarin in a formula that acts on multiple stages of melanin synthesis. Tranexamic acid blocks the bond between keratinocytes and melanocytes, interrupting the signal that leads to overproduction of melanin. Niacinamide interferes with the transfer of melanosomes to surface cells. Antioxidant components neutralize the oxidative stress that accompanies and amplifies the residual inflammatory response.
This second step overlaps with the first: Epicalm Plus and SPF 50 continue, while Lumicor is added to the evening routine.
Step 3: Continued sun protection (weeks 2–8)
Sunscreen isn't a complement to the post-laser protocol: it's an integral part of the result. Even after the skin has re-epithelialized, melanocytes remain in a state of increased reactivity for weeks. Any UV exposure during this period can negate the prevention efforts made in the previous phases.
The best sunscreen choice after CO₂ laser treatment is mineral filters (titanium dioxide and zinc oxide), which offer physical protection without chemical contact with regenerating skin. A SPF 50 face cream should be applied every morning as the last step in your routine, regardless of the season or weather.
For those who prefer a product that evens out skin tone during recovery, the SPF 50 tinted sunscreen with hyaluronic acid offers the same protection with a unifying effect that helps fade residual redness.
What to avoid after CO₂ laser
Direct sun exposure in the first 4–6 weeks, even partial and accidental.
Physical and chemical exfoliants (acids, scrubs, brushes) in the acute phase: the skin does not yet have an intact barrier and these products increase the risk of scarring and uneven pigmentation.
Manual removal of scabs: they fall off naturally and removing them early causes microtrauma resulting in localized melanogenesis stimulation.
Retinoids in the acute phase: Vitamin A derivatives are contraindicated during the active healing phase. Recovery can only occur after complete re-epithelialization and must be discussed with your doctor. To learn more about the difference between traditional and new-generation retinoids, you can read the article on tretinoin vs. new-generation retinoids.
Occlusive makeup in the first few weeks: it's best to opt for non-comedogenic products or, if necessary, a tinted cream with built-in sunscreen.
Frequently Asked Questions
When do spots appear after CO₂ laser?
PIH usually appears between the second and fourth weeks after the procedure, when re-epithelialization is complete and excess melanin becomes visible on the surface. In some cases, it can appear later, up to two months post-procedure, especially in darker skin types.
Is PIH after CO₂ laser permanent?
No. Post-laser PIH tends to resolve spontaneously over time, but without proper treatment, the process can take months or years. With a specific melanogenesis inhibition protocol and rigorous sun protection, regression is usually significantly faster.
Can I have CO₂ laser treatment in the summer?
Periods of high solar radiation significantly increase the risk of PIH. The ideal time to undergo CO₂ laser treatment is fall or winter, when the amount of environmental UV rays is lower and recovery can occur with less exposure. If the procedure occurs at other times, sun protection must be even more rigorous.
I had spots after a previous laser treatment. What can I do?
If PIH has already appeared, the protocol changes: it's no longer about prevention but about treatment. For more information on available options, you can consult the article on post-laser hyperpigmentation.
Does the post CO₂ kit already include everything ou need?
The Post-CO₂ Laser Facial Kit has been formulated to cover the three phases of the protocol: barrier repair, melanogenesis inhibition, and sun protection. It's a practical starting point, especially for those undergoing their first ablative treatment and looking for a structured protocol.
This article is written for informational purposes only. The information contained herein does not replace the advice of a dermatologist or aesthetician.