The problem of classic retinoids
Tretinoin has been considered the dermatological "gold standard" for the treatment of acne, photoaging, and hyperpigmentation for decades. However, clinical reality tells a different story: nearly 1 in 4 patients discontinues treatment due to side effects. Burning, erythema, scaling, and photosensitivity-these effects are not uncommon and are common in the first few weeks of use.
This guide analyzes the differences between tretinoin, retinol, and the new generation of retinoids particularly oleyl adapalenate with scientific data, explaining why seeking an alternative to tretinoin is not a matter of convenience, but a smart choice based on molecular biology.
How tretinoin works: mechanism and limitations
Tretinoin (all-trans-retinoic acid) is a first-generation retinoid that binds nonselectively to all three subtypes of nuclear retinoic acid receptors: RAR-α, RAR-β, and RAR-γ. This lack of selectivity explains both its potency and its tolerability issues.
When tretinoin binds to RAR-α and RAR-β receptors in basal keratinocytes and dermal cells, it triggers an inflammatory response that manifests as classic “retinoid irritation”: redness and scaling appear within the first 7–10 days, with peak symptoms occurring within the first 2–4 weeks.
Documented side effects of topical tretinoin (FDA drug labeling):
- Itching and skin pain
- Erythema (persistent redness)
- Flaking and peeling
- Intense skin dryness
- Photosensitivity: the skin becomes vulnerable to UV rays
- Instability to UV light: Tretinoin loses 80% of its activity in just 2 hours of sun exposure
A critical finding regarding photostability: spectrophotometric analyses show that tretinoin rapidly degrades in sunlight, effectively rendering it unusable in daytime formulations. This requires use exclusively in the evening, with all the resulting limitations on therapeutic adherence.
The phenomenon of "retinization"
The initial adaptation period—known as "retinization" or "retinoid uglies"—typically lasts 2 to 6 weeks. During this phase, many patients experience a paradoxical worsening of their skin before seeing any benefits. It is precisely during this time that the vast majority of treatment discontinuations occur.
Side effects
According to scientific literature, with 1% retinol, a full 47.3% of patients reported side effects at 12 weeks; with 0.025% tretinoin, the percentage drops to 12.6% but remains significant. The discontinuation rate due to irritation with traditional retinoids ranges between 15% and 25%.
Source: McDaniel et al., Journal of Cosmetic Dermatology, 2017.
Retinol: Popular, but not without problems
Retinol is the most widely used OTC retinoid in the world. Technically, it's a prodrug: the skin must convert it in two successive steps (retinaldehyde → retinoic acid) before it becomes biologically active. This mechanism has two important consequences.
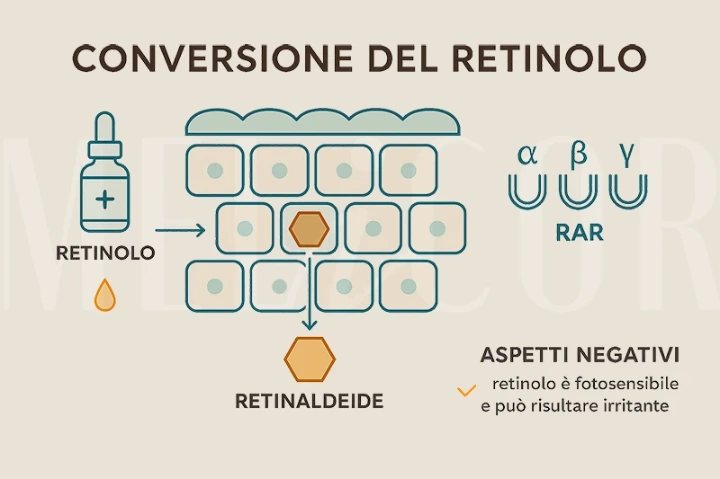
Pros: Gradual conversion reduces the intensity of acute irritation compared to direct tretinoin.
Cons: Conversion is partial and varies from individual to individual. Retinol is photosensitive and degrades rapidly if left unprotected. Most importantly, like tretinoin, it is not selective for RAR receptors—it acts on α, β, and γ—retaining its irritant potential.
The most worrying finding remains the incidence of side effects: nearly half of patients using 1% retinol report problems within 12 weeks. This makes retinol the worst in terms of tolerability among the retinoids compared in the literature.
The next-generation alternative: oleyl adapalenate
Oleyl adapalenate is a third-generation synthetic retinoid derived from naphthoic acid, obtained by esterifying adapalene with oleic alcohol. This chemical modification is not cosmetic: it radically changes the biological activity and tolerability profile.
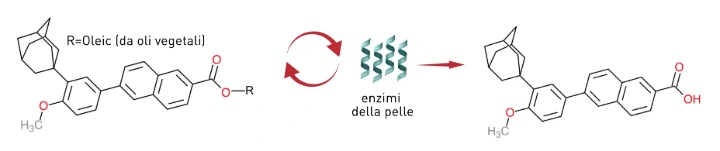
Enzymatic release of adapalene: the esterified form is cleaved by skin enzymes, releasing the pure active ingredient for a targeted and controlled action.
Receptor selectivity: the key to advantage
Unlike tretinoin and retinol, oleyl adapalenate selectively binds to RAR-γ receptors present in epidermal keratinocytes. RAR-α and RAR-β receptors—responsible for the inflammatory cascade that causes irritation—are essentially spared. The practical result is documented in the literature: 70% less erythema, scaling, and dryness compared to 0.5% retinol.
Source: Verschoore et al., British Journal of Dermatology, 1999.
Direct anti-inflammatory action
Adapalene possesses a property that neither tretinoin nor retinol possess: a direct anti-inflammatory effect. It inhibits lipoxygenase and arachidonic acid, reducing the production of pro-inflammatory leukotrienes and prostaglandins. This mechanism is particularly valuable in the treatment of post-inflammatory hyperpigmentation, where residual inflammation perpetuates melanin production.
Source: Sorg et al., British Journal of Dermatology, 2006.
Photostability: the advantage of daytime use
Oleyl adapalenate retains 90% of its activity after 24 hours of exposure to UV light. This allows, with adequate sun protection, even morning use, significantly increasing routine flexibility and therapeutic adherence.
Source: Thielitz et al., Photodermatology, Photoimmunology & Photomedicine, 2008.
Comparable efficacy with superior tolerability
A common objection to the adoption of new-generation retinoids is that they are "less effective." Data contradict this belief: in a randomized, multicenter study of 147 acne patients, 0.1% adapalenate gel achieved a 46% reduction in comedones versus 43% for 0.025% tretinoin, with a 44% vs. 40% reduction in inflammatory lesions, respectively. The efficacy was essentially equivalent, but the tolerability was significantly better.
Efficacy of adapalenate compared to tretinoin
Source: Shalita et al., Journal of the American Academy of Dermatology, 1996.
Comparison table: tretinoin vs. retinol vs. oleyl adapalenate
Scientific comparison based on clinical studies published in peer-reviewed journals.
Parameter | Tretinoin | Retinol | Oleyl Adapalenate |
Target receptors | RAR-α, β, γ | RAR-α, β, γ | RAR-γ selettivo |
Side effects (%) | 12,6% | 47,3% | < 5% |
Reducing irritation vs. retinol | Moderate | - | -70% |
Fotostabilità UV | - 80% in 2h | Instabile | ✓ −10% in 24h |
Direct anti-inflammatory action | No | No | ✓ Sì |
Daytime use possible | Not recommended | Not recommended | ✓Sì (con SPF) |
Discontinuation of treatment due to irritation | 15-25% | Very high | < 5%* |
Sensitive skin safety | Poor | Average | Excellent |
Availability in Italy | Prescription only | OTC | OTC (Lumicor) |
Sources: Shalita et al. (JAAD 1996), Verschoore et al. (BJD 1999), McDaniel et al. (JCD 2017), Thielitz et al. (PPAUM 2008).
Who should choose an alternative to tretinoin?
Tretinoin remains an effective drug for some specific indications, but there are patient profiles for which new-generation retinoids represent a clearly superior choice:
- Sensitive or reactive skin: irritation from tretinoin can worsen conditions such as rosacea, atopic dermatitis, or post-procedure skin.
- Post-laser hyperpigmentation treatment: The anti-inflammatory action of oleyl adapalenate prevents the risk of hyperpigmentation from trauma while promoting cell renewal. Read: Post-laser hyperpigmentation.
- Phototypes dark (III–VI according to Fitzpatrick): increased risk of post-inflammatory hyperpigmentation from retinoid irritation.
- Use during the day: the photostability of adapalenate allows for flexibility of use not possible with tretinoin.
- Patients who have already stopped taking tretinoin due to intolerance: switching to a RAR-γ-selective retinoid dramatically reduces the likelihood of experiencing the same problems again.
- OTC cosmetic use without a prescription: Oleyl adapalenate is available in cosmetic formulations without a prescription.
Oleyl adapalenate in practice: Melicor's anti-hyperpigmentation formula
Melicor has integrated oleyl adapalenate into Lumicor, an anti-hyperpigmentation cream that combines three complementary mechanisms of action in a single scientifically designed formulation:
- Oleyl adapalenate: accelerates the exfoliation of melanin deposited in the superficial layers, normalizes epidermal turnover, exerts a direct anti-inflammatory action.
- Cetyl tranexamate mesylate (highly bioavailable tranexamic acid): blocks pro-melanogenic signals at the level of keratinocytes, inhibits the transmission of melanogenic information from melanocytes.
- Tetraidrocurcumina (bioactive form of turmeric): directly inhibits tyrosinase, the key enzyme in melanin synthesis.
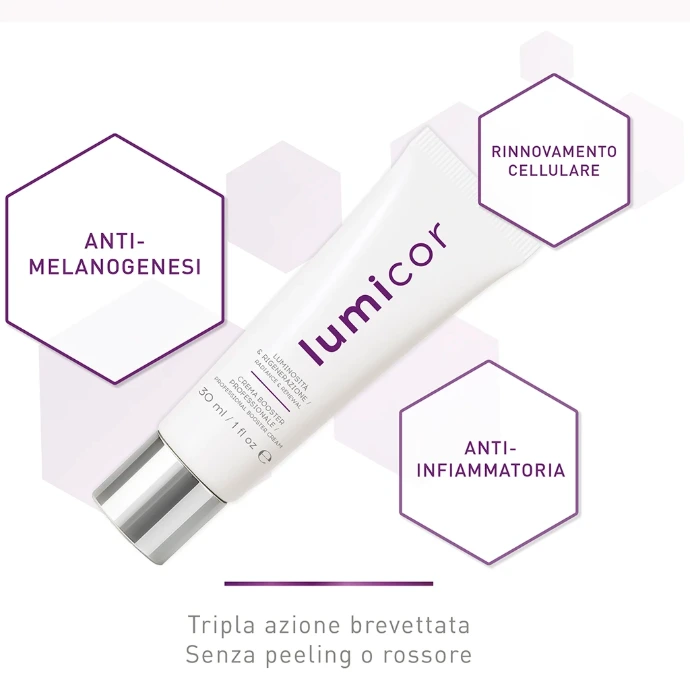
This "triple-action" synergy acts on three distinct levels of the pigmentation cascade: blocking production, interrupting transmission, and accelerating elimination. The combined effect is documented as superior to any single lightening agent.
Expected clinical results:
Weeks | Expected result |
1–2 | Skin adaptation, possible mild transient erythema |
3–4 | Beginning of improvement in tone, more uniform texture |
4–8 | Progressive reduction of blemishes, visible lightening |
8–12 | Maximum result: significant reduction of hyperpigmentation |
→ Discover Lumicor - anti-hyperpigmentation cream with tranexamic acid on melicor.it
Frequently Asked Questions (FAQ)
Is tretinoin more effective than adapalenate?
Clinical data show essentially equivalent efficacy for acne and hyperpigmentation, with adapalenate being significantly better tolerated. For photorejuvenation, tretinoin has been studied for longer; for post-inflammatory hyperpigmentation, adapalenate's anti-inflammatory action makes it preferable.
How long does it take to see results?
For hyperpigmentation: Initial improvements in tone at 3–4 weeks, visible reduction of dark spots at 6–8 weeks, maximum results at 12 weeks. For acne: reduction of blackheads at 4 weeks, improvement of inflammatory lesions at 6–8 weeks.
Can I use oleyl adapalenate if I have sensitive skin?
Yes, it is specifically designed for sensitive skin. RAR-γ selectivity eliminates the inflammatory cascade that causes irritation with traditional retinoids. The irritation-related discontinuation rate is less than 5%, compared to 15-25% for tretinoin.
Do I need to use sunscreen?
Absolutely yes, regardless of the type of retinoid. Retinoid accelerates cell turnover, making the surface layers temporarily more vulnerable to UV rays. SPF 50 is mandatory for the entire duration of treatment.
Can I use oleyl adapalenate during pregnancy?
No. Like all retinoids, it is contraindicated during pregnancy and breastfeeding as a precautionary measure (EMA/PRAC recommendations). Safe alternatives during pregnancy include azelaic acid, vitamin C, and niacinamide.
Related insights on melicor.it
- → Oleyl Adapalenate: Complete guide to third-generation retinoids
- → Post-laser hyperpigmentation: causes and scientific treatment
- → Tranexamic acid: the safest depigmenting agent on the market
- → Kligman's Formula: Composition and safe hydroquinone-free alternatives
- → Hydroquinone: Why it's banned in Europe and what safe alternatives exist
- → Lumicor: anti-hyperpigmentation cream without hydroquinone